
GLOBAL HEALTH: Blogs from Abroad
Allison Apfel, MD
RESIDENCY CLASS OF 2025
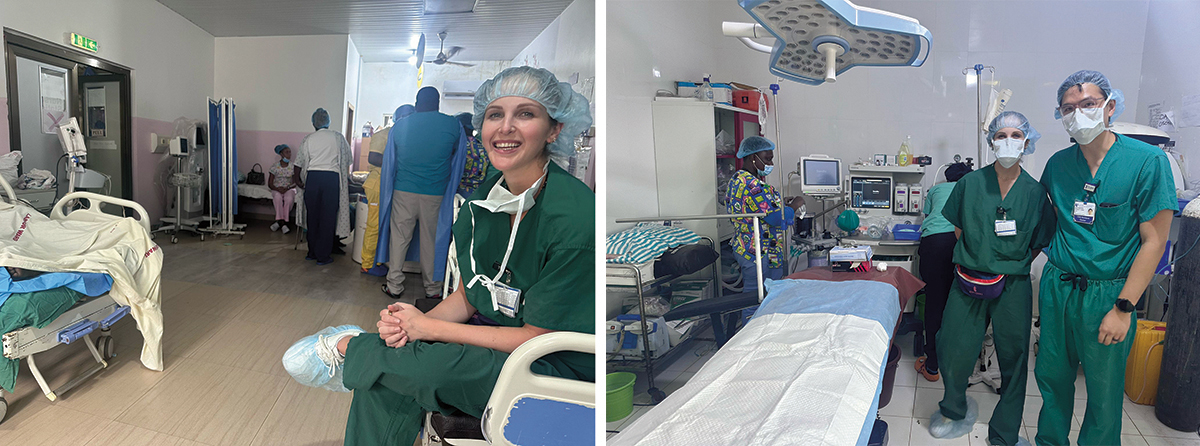
As I close out the last months of residency, I will remember my time in Accra as one of the most enjoyable and meaningful months of them all. It was a trip that I had looked forward to since my early years as an intern and CA1 – the opportunity to step outside of a familiar environment, experience a new culture, and learn about how anesthesia is practiced in a resource-limited setting. I wanted to see ways in which global health ventures could create a lasting impact on health care infrastructure through education and innovation in resource-limited areas. The experience exceeded every expectation.

We had the fortune of having Dr. Adeyemi Olufolabi as our mentor and host throughout the trip. As an obstetric anesthesiologist, his main focus is on improving obstetric anesthesia practices in the local hospitals there. He is specifically focused on improving epidural education and usage amongst providers. We spent a large majority of our time at the University of Ghana Medical Center, which is a newer hospital with somewhat more resources than other local hospitals, and we also got to visit more resource-poor hospitals. Dr. Olufolabi was basically a celebrity everywhere we went – Robert and I continued to be shocked at just how many people knew him. His popularity wasn’t just about familiarity, however; it is a testament to how passionate and dedicated he is to improving the anesthetic care in Ghana. His energy is contagious, and it is impossible not to be inspired by his commitment to making a lasting difference.
In addition to spending time on labor and delivery, Robert and I were able to be involved in several other types of environments such as the cardiac ORs, the ICUs, and the neonatal ICU. As a future pediatric anesthesiologist, being able to see the advancements made in key safety measures, such as enhanced monitoring practices, structured resuscitation training, and better infection control protocols in the neonatal ICU, was impressive.
Outside of our clinical time, Robert and I were able to experience the culture, warm hospitality, and vibrant energy of Ghana. We explored national parks, visited monuments and art museums, and took in the bustling markets. We also got to experience the local food; this turned out to be one of my biggest challenges of the trip, far more challenging than anything related to anesthesia. I learned that my taste buds were not fully equipped to handle the spice levels of Ghanaian food.
Overall, I think the most meaningful part of this experience was being able to see the importance and effectiveness of sustainable, education-driven change. Innovation doesn’t always need to come in the form of technology, and in Ghana, it is driven by a passion for improving patient care and outcomes. BP

Robert Chu, MD
RESIDENCY CLASS OF 2025

You are going to have fun. Welcome to Africa.” Those were the first words out of Dr. Olufolabi’s mouth as he embraced me in the muggy air outside of Kotoka International Airport in Accra. As we bounced down the road in the little black pickup truck that would be our ferry to so many adventures in Ghana, I had no idea exactly how much fun – and how many lessons, both in medicine and in life – I would experience over the coming four weeks.
The majority of our time in Ghana was spent at the University of Ghana Medical Center (UGMC), one of the country’s most advanced medical centers. While there, we worked alongside fellow trainees from the Ghanaian military and local hospitals, who welcomed us warmly into their operating rooms. Although UGMC is well-resourced compared to the other public hospitals we visited during our stay, some of the critical technological advancements that have made anesthesia so safe in the United States (and that we take for granted every day) were relatively new to their staff, so we spent time educating on and demonstrating the use of video laryngoscopes, neuromuscular blockade monitors, and ultrasound-guided access. Of course, we were also often humbled by the resourcefulness and skill of our colleagues in their ability to provide safe and effective anesthetics without consistent access to the latest technology that we enjoy in the U.S. I will never forget watching as one of the Ghanaian anesthesiologists placed the quickest central line I have ever seen - a blind IJ (!) on an 11-year-old (!) getting open heart surgery – faster than I could have even opened the kit.
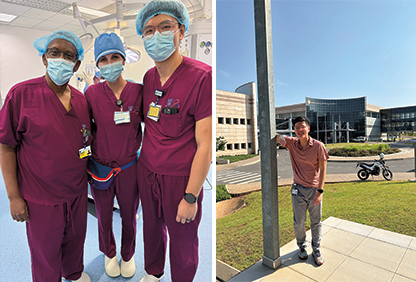
We were also able to participate in various educational activities at the School of Anaesthesia at Ridge Hospital in Accra, which was founded to provide education for much-needed anesthetists not only in Ghana itself, but also for visiting students from across Africa. We spent a day helping run an airway workshop for the trainees. Since general anesthesia is much less commonly used in Ghana compared to neuraxial or local techniques, the students really appreciated having hands-on education practicing with the donated laryngoscopes and mannequins in the school’s airway lab. As they honed their skills in bag-mask ventilation, supraglottic airway placement, and intubation, their good cheer and enthusiasm for learning were infectious; I couldn’t help but crack a smile as the students jokingly teased their friends or cheered them on after dunking a tube.
Finally, our month in Ghana served as a cultural experience that broadened our horizons and viewpoint on the world. From the chaotic streets of Makola Market to the sobering castles in Cape Coast that served as the final departure point for slaves headed to the New World, Ghana amazed us daily with its historical richness and its people’s fierce pride in their country and culture. Never have I before encountered a group of people as friendly, open, and willing to share with total strangers. One day, Dr. Olufolabi brought us along to a funeral (which are, to put it lightly, a big deal in Ghana), where, despite not knowing anyone in attendance, we were feted with seats of honor and plied with more delicious food and drink than we could handle. Such hospitality was the rule, not the exception, wherever we went, in a way that made the whole country feel like one tight-knit community. In the end, it was this sense of togetherness – among anesthesiologists, health care workers, and most importantly just people living in a society – that was the most valuable takeaway from my time abroad. So yes, Dr. Olufolabi, I did have fun in Ghana. But I’d like to think that I left a little bit wiser, and better, as a physician and a person. BP
